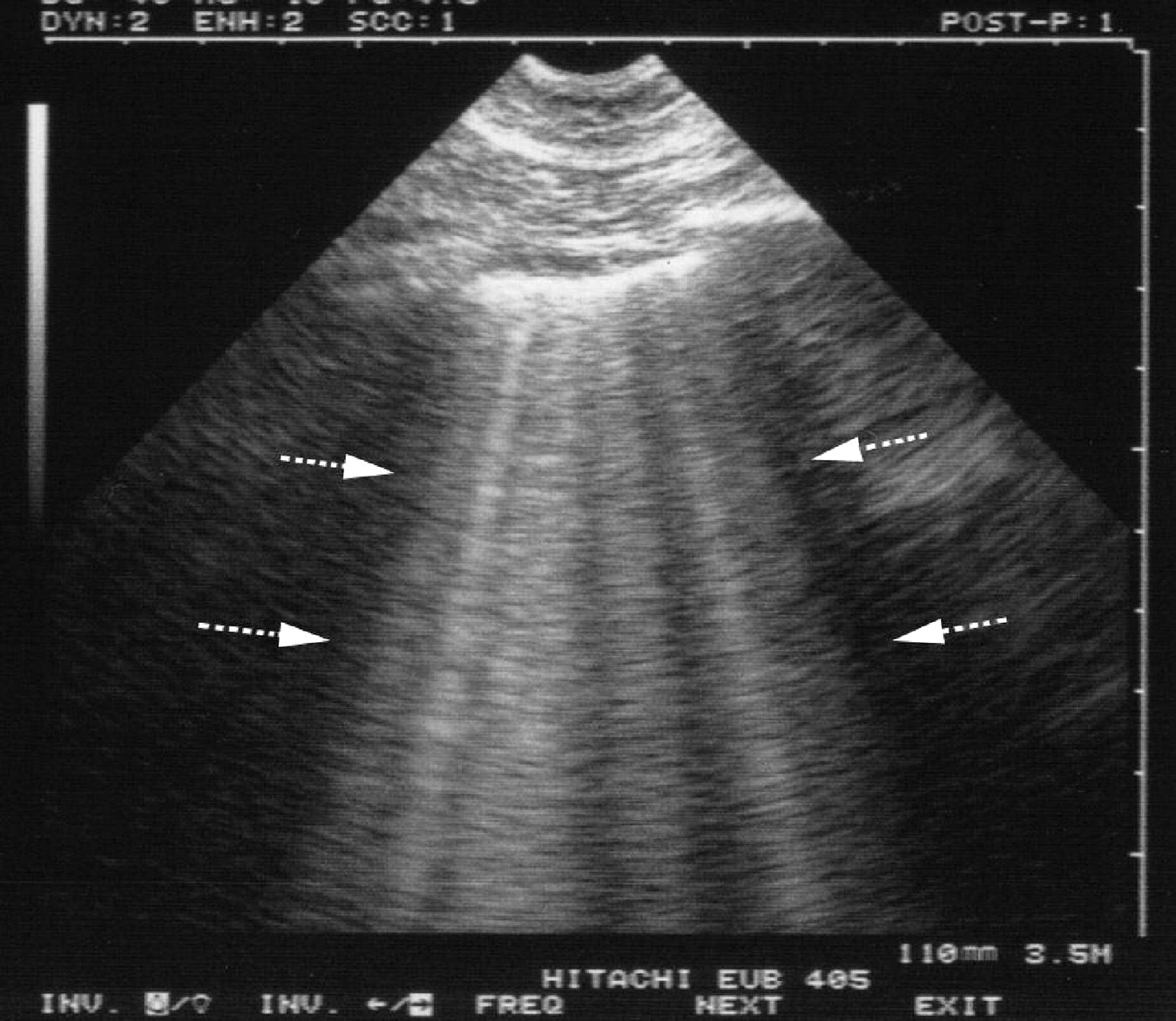 
Risk factors for the development of cardiogenic pulmonary edema include heart disease, high sodium meals and overzealous fluid therapy (crystalloid or colloid).Risk factors for the development of non-cardiogenic edema include accidental exposure to a trigger or severe underlying illness. In either case, signs of pulmonary edema include tachypnea and respiratory distress. electric cord injury, upper airway obstruction or seizures) or the patient may be hospitalized with serious illness. In animals with non-cardiogenic pulmonary edema, they may have had an event, that is a known trigger of non-cardiogenic pulmonary edema (i.e. Cats with heart failure may have had no premonitory signs other than acute onset of respiratory distress. Other historical complaints for cardiogenic pulmonary edema include tachypnea or orthopnea, respiratory distress and coughing. In many dogs with cardiogenic pulmonary edema there is a history of a heart murmur due to endocardiosis. Common veterinary causes of non-cardiogenic pulmonary edema include upper airway obstruction (transient), electric cord injury, and sepsis/acute respiratory distress syndrome (ARDS). Non-cardiogenic edema results from decreased colloid osmotic pressure or altered vascular permeability in the pulmonary capillaries. Common causes of left-sided heart failure in small animals include dilated cardiomyopathy, acquired mitral valve regurgitation, and hypertrophic cardiomyopathy. Cardiogenic pulmonary edema results from increased pulmonary capillary hydrostatic pressure caused by left-sided heart failure. Pulmonary edema is generally divided into cardiogenic and non-cardiogenic forms based upon the etiology. 
Increased capillary hydrostatic forces will result in a low protein edema fluid while lowered colloid osmotic forces will promote a high protein edema fluid. Pulmonary edema forms when there is an alternation in the balance of Starling forces (hydrostatic and colloid osmotic) between the interstitium and pulmonary capillary beds that favors increasing filtration to the interstitium. Pulmonary edema may range from clinically insignificant to life-threatening. Any duplication or distribution of the information contained herein is strictly prohibited.Pulmonary edema is defined as the accumulation of abnormal amount of extravascular lung water. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language. Links to other sites are provided for information only – they do not constitute endorsements of those other sites. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. This site complies with the HONcode standard for trustworthy health information: verify here. 
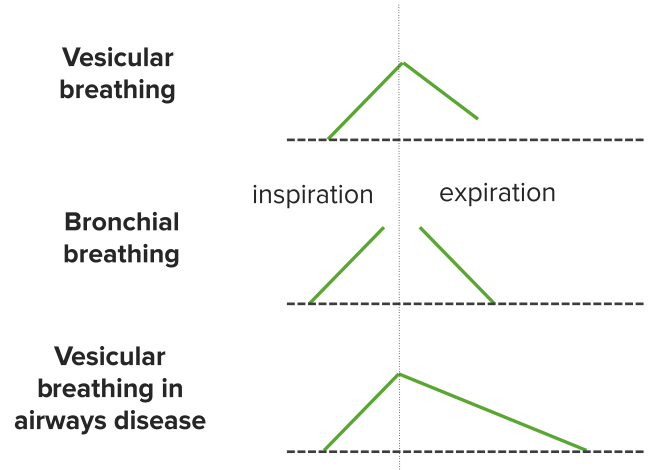
Learn more about A.D.A.M.'s editorial policy editorial process and privacy policy. is among the first to achieve this important distinction for online health information and services. follows rigorous standards of quality and accountability. is accredited by URAC, for Health Content Provider (URAC's accreditation program is an independent audit to verify that A.D.A.M. Wheezing and other abnormal sounds can sometimes be heard without a stethoscope.Ī.D.A.M., Inc. They are most often heard when a person breathes out (exhales). High-pitched sounds produced by narrowed airways. Usually it is due to a blockage of airflow in the windpipe (trachea) or in the back of the throat. Wheeze-like sound heard when a person breathes. They occur when air is blocked or air flow becomes rough through the large airways. Rales can be further described as moist, dry, fine, and coarse. They are believed to occur when air opens closed air spaces. They are heard when a person breathes in (inhales). Small clicking, bubbling, or rattling sounds in the lungs. There are several types of abnormal breath sounds. Over-inflation of a part of the lungs ( emphysema can cause this).Air or fluid in or around the lungs (such as pneumonia, heart failure, and pleural effusion).Using a stethoscope, the health care provider may hear normal breathing sounds, decreased or absent breath sounds, and abnormal breath sounds. Normal lung sounds occur in all parts of the chest area, including above the collarbones and at the bottom of the rib cage. The lung sounds are best heard with a stethoscope.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
